
Article
Case report : perforated appendix within a right inguinal hernia sac (Amyand’s hernia)
Introduction:
A normal or inflamed vermiform appendix that is found inside an inguinal hernia sac is called Amyand’s hernia, in honour of the surgeon Claudius Amyand who was the first to report this rare entity in the eighteenth century.
Amyand’s hernias usually present on the right side as this is the normal anatomic position of the appendix. In rare cases associated with situs inversus, malrotations of the intestines and mobile caecum, an Amyand’s hernia may appear on the left side.
The clinical presentation of an Amyand’s hernia usually mimics a strangulated inguinal hernia and therefore the vast majority of these cases are not diagnosed preoperatively. In fact there are very few cases of preoperatively diagnosed Amyand’s hernias in literature .
The aim of this report is to present a rare and very interesting case of a clinically incarcerated inguinal hernia which proved to be an Amyand’s hernia intraoperatively.
Description of Case:
A 60 year old male patient presented to our emergency department complaining of a painful swelling in the right inguinal area which started three days ago. The pain was moderate and there was no associated signs of intestinal obstruction . On examination the swelling was tender and warm . The swelling was irreducible though the patient had a medical history of reducible swelling in the same region. The past medical history was not significant and the patient had no history of associated co-morbidity. Pain onset was sudden and involved only the right inguinal area. Abdomen was found to be soft with no features of peritonitis. No significant clinical findings were revealed by digital rectal examination and examination of the scrotum . Body temperature was slightly increased. Laboratory findings included elevated inflammation markers: White Blood Cell count: 14.9 x 10^g/L with granulocytes of 83.3% . Urine examination was normal, so a provisional diagnosis of right side strangulated inguinal hernia was made. The differential diagnosis of the inguinal mass included local abscess, incarcerated hernia or combination of both disorders. Ultrasonic examination was requested to rule out other pathologies. It confirmed the presence of hernial sac.
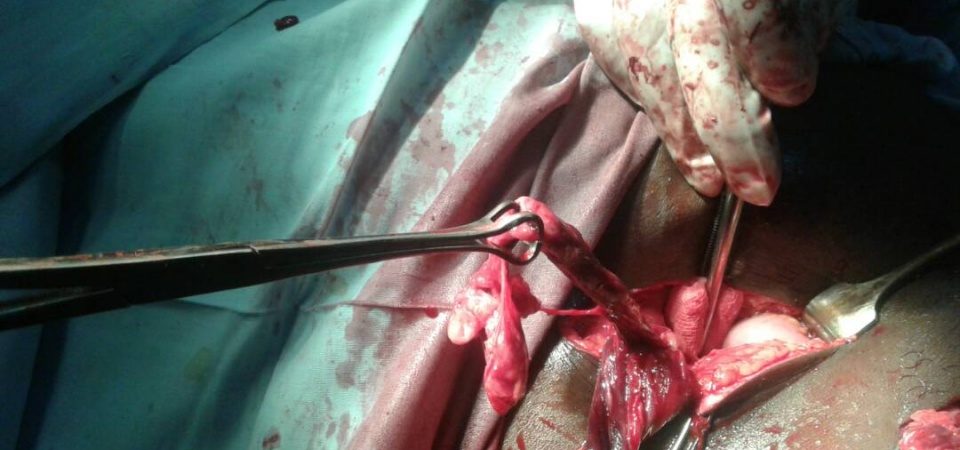
The patient was reassured and prepared for emergency surgery. The inguinal canal was explored taking care not to injure the congested and fragile structures . All adhesions were released and the severely inflamed hernial sac was opened. It contained part of the greater omentum enveloping a perforated appendix , necrotized tissues and pus
. Mass reduction of the contents without dissecting the layers of the inflamed omentum would have resulted in missing the main pathology with subsequent disastrous consequences for the patient. The perforated appendix was relatively long with its base and the caecum laying intra-abdomen .This made appendectomy difficult through the inguinal incision. Another incision (Grid-Iron) had to be made in the right iliac fossa to excise the perforated appendix. A suction drain was put in the right iliac fossa before closing this incision. The redundant hernia sac was ligated then resected through the herniotomy incision. The posterior wall of the inguinal canal was strengthened with nylon monofilament darn repair. No mesh was placed in to avoid postoperative complications such as wound infection.
It is important to state that we did not consider laparotomy to be necessary at the first place because of the fact that the sepsis was limited within the inguinal area and the pre-operative presentation of the patient was not indicative of peritonitis .
The drain was removed on day three post-operatively and the patient was discharged home five days after surgery.
Discussion:
The probability of an individual to have acute appendicitis at some point in his life is about 8%1. The incidence of a non-inflamed appendix within adult inguinal hernias is about 1%. The case of an inflammed, perforated appendix or periappendicular abscess within an inguinal hernia in adults is much lower and accordingly to different studies ranges between 0.13% and 1%2. In a 2003 study by C. D’Alia et al only one case of acute appendicitis within an inguinal hernia in 1.341 repair operations was described.
The underlying mechanisms that can lead to acute appendicitis within an Amyand’s hernia include the reduction of the appendix’s blood supply due to adhesions that may cause non-reducibility of the hernia and compression in the external ring originating from increases in intra-abdominal pressure. These factors lead to recurrent inflammation and bacterial overgrowth.
An Amyand’s hernia is virtually always diagnosed intraoperatively . Computer tomography can be diagnostic, however it is rarely used due to the fact that such a hernia usually mimics either a simple reducible or an incarcerated inguinal one and is therefore admitted for elective or emergency surgery respectively, without using any prospective imaging techniques.
Unlike other inguinal hernias containing bowel that may cause ileus, an Amyand’s hernia usually appears without signs of obstruction and inflammation markers usually stay within normal range. The differential diagnosis may include strangulated hernia, Richter’s hernia, orchitis, omentocele, inguinal lymphadenitis, epidydimitis and hemorrhagic testicular tumor.
The management of Amyand’s hernias is still a subject of debate and should be individualized depending on appendix’s inflammation stage , presence of abdominal sepsis, operative findings and co-morbidity factors. The Losanoff-Basson classification

offers a satisfactory guidance system. In type I, hernia reduction with mesh repair and appendectomy (unless contraindicated) is the treatment of choice. In Type II Appendectomy through herniotomy with primary repair of hernia with Bassini or Shouldice technique (no mesh) is proposed. In type III, a laparotomy, appendectomy and peritoneal lavage and subsequent hernia repair without mesh is indicated. Finally in type IV, a laparotomy in terms of identification and treatment of this pathology should be performed. Appendectomy and hernia repair without mesh should follow. Most surgeons agree that the presence of acute appendicitis (Losanoff-Basson type II-IV) within a hernia should be a contraindication for the use of synthetic meshes or plugs. However a point of disagreement is whether or not to perform an appendectomy in a case of a Losanoff-Basson type I Amyand’s hernia (normal appendix within inguinal hernia). The decision should be based on factors like the patient’s age, the size and anatomy of the appendix, the side in which the hernia occurs and finally the extension of the intraoperative manipulations that can by themselves trigger an inflammatory process.
In our case, we dealt with a type II Amyand’s hernia with a perforated appendix and no signs of abdominal sepsis, never the less we proceeded with an appendectomy through a right iliac fossa Grid – Iron incision because appendectomy through the herniotomy incision was technicaly difficult as explaind earlier. This was follwed by primary repair of the hernia without the use of any synthetic mesh or plug. The outcome was excellent and the patient was discharged without any complications, but later he developed post operative wound infection which responded well to dressing and antibiotics.
* In terms of statistical analysis, our surgical clinic provides services to a population area of 100,000. A mean of 100
Conclusion:
Amyand’s hernia is a rare type of inguinal hernia which is difficult to diagnose preoperatvily. It can sometimes lead to serious and life-threatening complications due to peritoneal spread of the septic process and therefore operating surgeons should be well trained to accurately identify the contents of a hernial sac and to avoid mass reduction .
References:
1. Sengul I, Sengul D, Aribasw D. An elective detection of an Amyand's hrrnia with an adhesive caecum to the sac: report of a rare case. N Am J Med. SCI. 2011;3:391-393
2. Ryan WJ. Hernia of vermifrorm appendix. Ann Surg.1937;106;135-139
Author:
Dr. Tayseir Hamid Moh.
Colonel , Medical corps, Sudanese Armed Forces.
General surgeon, Omdurman military hospital.
Forward surgical team , field hospital , Khokha.
Graduated (MBBS) from Dr.Ambedkar medical college, Bangalore university , India.
MD (GENERAL SURGERY), Gezira university, Sudan.
E-mail: [email protected]
Date: 07/25/2018










