
Article: Alexander Popov, Igor Yakirevich
COMPLEX TREATMENT OF CRUSH SYNDROME IN FIELD HOSPITAL IN EMERGENCY AREA
From the department of anaesthesiology, resuscitation and intensive care of the field hospital of Central Airmobile Rescue Team of EMERCOM of Russia
INTRODUCTION
The problem of crush syndrome management still remains urgent over a period of two hundred years. Medical consequences of earthquakes and medical organization of emergency response do not have a full scientific development so far. The technology of medical aid rendering in case of the extrication of a victim with crush syndrome who is trapped under the debris is described in literature but there is no common opinion concerning the tactics and continuity of the treatment of such pathology in emergency area in case of mass medical losses. It concerns the issues of management and prevention of ishaemic endotoxicosis during extrication, rendering of qualified medical aid in field hospitals in emergency area, surgical tactics, infusion therapy methods and validity of active detoxification methods application at the stages of medical evacuation before admission of victims to specialized medical facilities outside emergency area.
MAIN SECTION
Victims often lose their lives under the debris (isolation phase) waiting for rescuers and physicians. Due to the developed ishaemic endotoxicosis the mortality rate at the stages of medical evacuation is high as well. Our practical experience enables us to draw the conclusion that treatment tactics and crush syndrome prevention should be flexible and adapted to the conditions of a certain emergency taking into account the scale and structure of medical losses, disaster nature and geographic location. The US National Guard renders the first medical aid by means of rapid helicopter evacuation of a victim from emergency area to a specialized medical facility. In emergency area paramedics render medical aid essential for the support of vital organs. Such tactics is adhered to if air evacuation transport is ready and if there is no delay in victim’s extrication. We applied it practically in Indonesia (a 8.0 earthquake, 2008, Nias Island, Indonesia) in cooperation with the air forces of the US Navy Marines. The victims were evacuated to the USNS Mercy (T-AH-19) hospital ship only after the complex of intensive therapy and the stabilization of their condition in the field hospital of EMERCOM of Russia was performed.
In case of mass medical losses and lack of triage of victims according to their condition severity these conditions are absent. Such victims should be rendered medical preventive measures on site in emergency area. Our experience enables us to conclude that basic anti shock measures and victims’ condition stabilization should be performed at the extrication site and at the stages of evacuation. Evacuation delay will be well-grounded due to objective reasons. In conditions of emergency it will enable to reduce ungrounded mortality rate at the evacuation stages.
It is not possible to perform quick and targeted evacuation to specialized medical facilities from emergency area during the first several days. In our opinion the concept concerning immediate evacuation of victims with severe traumas to a hospital base in conditions of mass medical losses is impracticable. This conclusion is corroborated by our practical experience in emergency response during the earthquakes in Turkey (2001), Iran (2003), Indonesia and Pakistan (2005), China (2008) and Haiti (2010). Arising panic and stress conditions (stupor and feverish activity) concerns not only the victims themselves but a part of survived local medical personnel who are practically not always able to take charge. It can be explained by the fact that during the first days there is nobody to perform the triage according to the condition severity and in fact there is no possibility to transport the victims to a specialized medical facility from emergency area. It is caused by the destruction of roads, air fields, hospitals and remoteness of specialized medical facilities.
Rescued victims who were evacuated from emergency area are concentrated at air fields and in refugee camps. The lack of food and water in supply, high concentration level of victims and refugees have a negative impact on the quality of medical aid. In such situation it is impossible to discuss any qualified medical aid and rendering specialized medical aid all the more. According to the literature analysis and our practical experience we came to the conclusion concerning the lack or impossibility of carrying out the full complex of preventive medical measures among the victims with crush syndrome at the stages of evacuation to a specialized medical facility. It is caused by a range of objective factors:
- Stupor, panic and reactive psychosis, as the result – full apathy to what is going on among the survived medical personnel and affected population.
- Warning and communications systems are damaged.
- Local emergency management agencies are not prepared for rigorous management, disaster scale assessment, evaluation of forces and resources mobilization.
- Infrastructure is damaged (hospitals, roads, air fields). It causes difficulties for carrying out SAR operations and victims’ evacuation.
- Lack of victims’ triage, mass type of affection of traumatic nature.
- Public health facilities are damaged, the usual system of medical aid rendering to the population does not function properly, and new unusual problems emerge.
- It is impossible to use small aircraft to a good quality (only helicopters).
- There is no “targeted” evacuation, victims’ concentration in refugee camps results in the increase in the number of evacuation stages and the loss of time accordingly.
- Complicated geophysical environment and continuous aftershocks.
- Ethnic and religious factors and traditions of the local population.
Intricate climatic conditions have negative impact as well: tropical and subtropical zones, temperature difference up to 30o per 24 hours, highland conditions and air humidity up to 100%; continuous seisms; dangerous epidemiological conditions, caused by damaged sewing systems, emission and spread of industrial and domestic waste.
In our paper we recount our opinion concerning medical and preventive complex which is carried out to the victims with crush syndrome directly in emergency area.
OBJECTIVE OF STUDY
Generalization of the experience of complex treatment of the victims with crush syndrome with the application of membranous plasmapheresis without apparatus (MPPA) in the field hospital of EMERCOM of Russia in case of elimination of medical consequences of earthquakes (Indonesia and Pakistan, 2005, China, 2008, Haiti, 2010).
MATERIALS AND METHODS OF STUDY
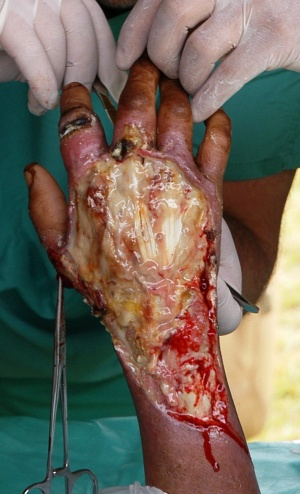 Figure 1: Crush syndrome of a hand after initial surgical debridement (Pakistan, 2005).
Figure 1: Crush syndrome of a hand after initial surgical debridement (Pakistan, 2005).
The complex of medical and preventive measures carried out by the medical service of the field hospital of EMERCOM of Russia for the victims with crush syndrome in emergency area comprises of 2 stages.
FIRST STAGE
The first stage is performed directly by the physician of USAR team on the site of victim’s extrication from under the debris:
- Intravenous anaesthesia (intramuscular): 50% analgin (2,0 ml), baralgin (5,0 ml); buprenorphine – unit-dose syringe; 1-2% promedol(1,0 ml).
- Intravenous introduction of hormonal agents: prednisolone – 5-30 mg per 1 kg of body mass.
- Infusion and alkalizing therapy including introduction of fluid by means of probe or drinking (on condition that acute abdomen and bladder injury were eliminated). Infusion therapy should include 4% solution of sodium hydrogen carbonate for the purpose of prevention of acidosis and acute renal failure development.
- Tourniquet application before the extrication from under compression with the subsequent tight strapping and removal of tourniquet. Tourniquet application will prevent reperfusion into the compressed extremity and enable to maintain stable haemodynamics at the moment of extrication and transportation to the field hospital.
- Transport immobilization is performed with transportation splints of any type (pneumatic splints are preferable due to their double function – compression creation and stable extremity fixation).
- Ischemic tissue is cooled regionally with cooling foil, chemical cooling agents and hot-water bags filled with ice.
- Immediate evacuation from the extrication site to the field hospital.
- Amputation under pressure is performed in case of an evident threat to the lives of the victim and rescuers during the extrication (structure fragments collapse).
SECOND STAGE
The complex is performed in the operating room and anaesthesiology and resuscitation unit of the field hospital:
- Anaesthesia. Elimination or reduction of painful impact and stressful situation. Narcotic analgesic and tranquilizers were used. Intravenous anaesthesia: 1-2% promedol- 1,0 ml in combination with dormikum (2,5 mg) or 0,025% droperidol (2,0 ml) and 0,005% fentanyl (2,0 ml) (talamanal).
- Infusion and alkalizing therapy. Infusion and alkalizing therapy is performed including fluid introduction by means of probe or drinking (on condition that acute abdomen and bladder injury were eliminated). Restoration of acid-base balance and water-electrolytic blood composition, hemodilution support with 25-30% haematocrit. 4% solution of potassium hydrogen carbonate (400-600 ml) for the prevention of acidosis and acute renal failure development. Infusion therapy volume was 7-8 liters per 24 hours.
- Blood coagulation system correction. Heparin (2 500 units) 4 times per 24 hours, rheopolyglucin, trental.
- Complex detoxification. Application of active methods of homeostasis correction.
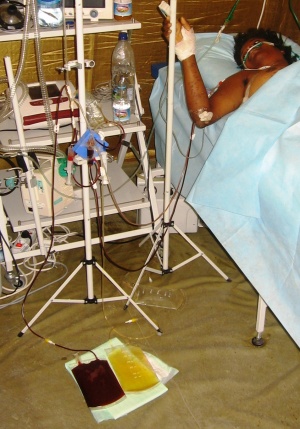 Figure 2: MPPA procedure in the field hospital in Haiti (2010).
4.1.Single-needle membranous plasmapheresis without apparatus (MPPA) was performed using plasmafilters “ROSA” with the removal of up to 70% of plasma circulation volume with hypervolemic (+20%) combined substitution. 2±1 procedures were carried out to each patient. On the average 70±10% of plasma circulation volume were removed per 1 procedure with hypervolemic (+20%) combined substitution. The volume of removed plasma was calculated individually for each patient – from the average volume (20-50% of plasma circulation volume) to plasma exchange. Procedure frequency – 1 time per 24 hours. Plasma circulation volume was calculated according to the generally accepted scheme. Substitution agents: crystalloids (0,9% NaCl or Ringer solution), hydroxyethylized starches (6% Voluven, 6% HAES, Haes-steril 10%), proteins (6-10% albumen). Fresh frozen plasma (FFP) and perftoran were not used due to the complexities in their transportation and storage in emergency area. The first MPPA procedure was performed within 2 hours after the victim’s extrication from under the debris. MPPA procedure duration – 60-120 minutes. 1,5% Reamberin solution infusion was carried out after the MPPA procedure in order to increase the detoxification effect (2-7 ml per 1 kg of victim’s body mass).
Figure 2: MPPA procedure in the field hospital in Haiti (2010).
4.1.Single-needle membranous plasmapheresis without apparatus (MPPA) was performed using plasmafilters “ROSA” with the removal of up to 70% of plasma circulation volume with hypervolemic (+20%) combined substitution. 2±1 procedures were carried out to each patient. On the average 70±10% of plasma circulation volume were removed per 1 procedure with hypervolemic (+20%) combined substitution. The volume of removed plasma was calculated individually for each patient – from the average volume (20-50% of plasma circulation volume) to plasma exchange. Procedure frequency – 1 time per 24 hours. Plasma circulation volume was calculated according to the generally accepted scheme. Substitution agents: crystalloids (0,9% NaCl or Ringer solution), hydroxyethylized starches (6% Voluven, 6% HAES, Haes-steril 10%), proteins (6-10% albumen). Fresh frozen plasma (FFP) and perftoran were not used due to the complexities in their transportation and storage in emergency area. The first MPPA procedure was performed within 2 hours after the victim’s extrication from under the debris. MPPA procedure duration – 60-120 minutes. 1,5% Reamberin solution infusion was carried out after the MPPA procedure in order to increase the detoxification effect (2-7 ml per 1 kg of victim’s body mass).
4.2.Infusion forced diuresis. Application of artificial stimulation of diuresis at the diuresis level of 300 – 500 ml per hour. In case of preserved diuresis (more than 20 ml per hour) 15% mannitol solution infusion was used at the speed of 10 ml per hour. In contrast to mannitol furosemide was used accompanied with abrupt decrease of diuresis and eliminated hypovolemia.
4.3.Enterosorption with carbonic sorbent together with cleansing enemas.
- Prevention and elimination of purulent and septic complications. Antibacterial therapy with broad-spectrum medications (cephalosporins and metronidazole). Nephrotoxic and hepatotoxic medications should be avoided.
- Initial surgical debridement. Initial surgical debridement, opening and drainage of haematomas, necrotic mass zones (necrotic zones) excision, fracture reduction are carried out using general anaesthesia. Premedication was performed directly in the preoperative room 5-10 minutes before the surgery. It consisted of intravenous introduction of promedol and atropine (age-dependent dosages). For introduction to anaesthesia ketamine (4-10 mg per 1 kg of body mass) in combination with seduxen were used intravenously. For maintaining anaesthesia: fractional introduction of fentanyl (0,1 – 0,2 mg), ketamine (2 – 4 mg/kg) and seduxen (0,25 mg/kg). Myoplegia: arduan (0,03 mg/kg per hour). System haemodynamics (heart rate, blood pressure, ECG), breathing (respiratory rate, Sat O2) were continuously controlled with the monitors and pulse oxymeters in the operating room as well as in the resuscitation unit. Total intravenous anaesthesia was performed in combination with artificial pulmonary ventilation in normal ventilation mode. Intramuscular anaesthesia was carried out with ketamine (4-10 mg/kg) and seduxen (0,25 mg/kg). No complications were observed during anaesthesia.
Extremity (extremity part) amputation indications were full mechanical destruction of extremity and ischaemic necrosis.
No surgical debridement was performed. It is caused by a range of factors including the danger of profuse plasmorrhea, further tissues infection and sepsis development, impossibility of efferent therapy.
- Cooling of ischaemic tissue with cooling foil, chemical cooling agents or hot-water bottles filled with ice.
- Transport immobilization before evacuation to a specialized medical facility. Immobilization is performed with transport splints of any type; pneumatic splints are preferable due to their double function – compression creation and stable extremity fixation.
RESULTS
This complex of medical preventive measures was used among 38 (19 males and 19 females) victims with crush syndrome in the field hospital of EMERCOM of Russia in Pakistan, China, Indonesia and Haiti (earthquakes of 7,0 – 8,5 magnitude on the Richter scale).
Victims’ age – from 15 to 60 (average age - 34,5±4).
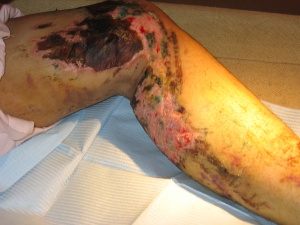 Figure 3: The results of the complex treatment. Granulation can be seen on a crushed extremity.
Figure 3: The results of the complex treatment. Granulation can be seen on a crushed extremity.
Extrication period: up to 48 hours – 25 persons, more than 72 hours – 13 persons. All victims were in the state of apathy, conscious level was 12±2 according to Glasgow coma scale. During the examination of compressed extremities pathological changes were noted: from hyperaemia to cutaneous surfaces necrosis, intracutaneous and subcutaneous haematomas. Tubular bones fractures were observed among 14 victims. Pathological changes of tissues up to necrosis with purulent and septic complications were observed among 17 victims. 1 victim had a totally crushed foot. The movement in the joints of affected extremities was highly limited due to the compression along with a growing edema. The pulsation in the distal parts of arteries was weak or uncertain. The loss of sensitivity in the compression zones and lower was observed among 23 victims. Their severity condition according to Glasgow coma scale was 12±1, according to APACHE II - 29±4. Tendency towards hypotension and tachycardia, hyperthermia in the range of 37,8 - 39°С, increase of short breath were observed. During the admission of the victims with crush syndrome: Hb 95±3,7 g/l, Ht 42±2,1 %, ESR 36±5, white blood cell count left shift, total protein 54,8±3,1millimole\l, urea13,0±1,7 millimole\l, blood glucose 6,8±0,6 millimole\l, Na 137±2 millimole\l, plasma potassium 6,5±0.2 millimole\l. Myoglobin level was not tested due to the lack of special laboratory equipment. All above-stated factors indicated the development of endogenous intoxication syndrome development. Field hospital admission period was from several hours up to 5 days.
Positive clinical effect was observed among all 38 victims who got this medical preventive complex. Haemodynamics characteristics stabilization: tachycardia decrease, arterial and central venous pressure normalization were observed in 28±6 hours. Increase in daily diuresis up to 1200±100 ml/day was observed in 18±8 hours. Laboratory tests after complex therapy in the field hospital: Hb 101±3,2; Ht 28±1,8; total protein 60,1± 2,7 millimole/l; urea 8,7±1,5 millimole/l; plasma potassium 3,7±0,1 millimole/l.
All victims were evacuated to specialized medical facilities (the distance from emergency area was up to 200 km) accompanied by physicians. No mortality was observed during their admission in the field hospital and at the stages of evacuation.
CONCLUSION
The tactics of treatment of the victims with crush syndrome should be flexible and adapted to each certain emergency. MPPA application enables to reduce the rate of complications and mortality. MPPA is a method of choice of extracorporal homeostasis correction among the victims with crush syndrome in field hospitals in emergency area. We suggest that in case of mass medical losses during emergency response the volume of qualified medical aid should be expanded by means of specialized medical aid (efferent therapy methods) in conditions of field hospitals. The application of MMPA at the early stage of medical aid rendering in emergency area enables to reduce the development of severe endotoxicosis types which result in multiorgan failure syndrome and acute renal failure development.
Author’s address
EMERCOM of Russia, State Central Airmobile Rescue Team
Mendeleev st. 12
140180 Zhukovsky, Moscow Region, Russian Federation
[email protected]
Date: 09/24/2018
Source: Medical Corps International Forum 1/2013











