
Article
Stress fracture of the radius as a result of kettlebell training – A case report
Outpatient Department (Head: C. Holtherm, MD, LtCol, MC) of the Bundeswehr Center of Sports Medicine, Warendorf¹ (Head: A. Lison, MD, Col, MC) and Center of Radiology and Nuclear Medicine, Ahlen/Beckum/Warendorf² (Head: K. A. Balhorn, MD, and Colleagues)
Katrin Bender¹, Christoph Holtherm¹, Karl A. Balhorn², Andreas Lison¹
Wehrmedizinische Monatsschrift 2016; 60(7): 218 - 222
Background
A stress fracture is a common response of the skeletal system to overloading. This response can range from bone marrow edema to a complete fracture and most frequently occurs in the lower extremity. Stress fractures of the bones of the upper extremities and thorax are less common because these bones are biomechanically exposed to considerably lower loads than weight-bearing bones. For this reason, these fractures are often not considered as a differential diagnosis especially during initial assessment.
Case presentation. We report the case of a 42-year-old male soldier who sustained a stress fracture of the distal radius during intensive kettlebell training.
Discussion and conclusions. We describe extrinsic and intrinsic risk factors that led to a stress fracture in the patient presented here and depict potential clinical signs and symptoms. In addition, we discuss radiological imaging modalities and their sensitivity and specificity for this injury pattern. Both conservative and surgical treatment options are available to physicians and patients. The choice of treatment depends on the severity, cause and site of injury. We provide information that may help unit physicians treat and counsel patients in order to help them prevent stress fractures. In addition, we attempt to increase awareness of stress injuries as a differential diagnosis.
Key words. Stress fracture, fatigue fracture, upper extremity, overloading, kettlebell training
Introduction
Stress fractures in soldiers, also known as march fractures, were originally described in 1855 by BREITHAUPT, a Prussian military physician. [1] Stress or fatigue fractures are still seen today by unit physicians in routine clinical practice and result when the musculoskeletal system is overloaded. These fractures most commonly occur in the metatarsal bones and less frequently in the tibia and fibula. In the majority of cases, the lower extremity is affected. Upper-extremity and rib stress fractures account for less than 10% of the cases. [2]
Kettlebell training has become very popular in the fitness community. A kettlebell resembles a cannonball with a handle and is used for free-weight workouts. With an offset center of mass, this piece of fitness equipment is particularly useful for training not only specific muscles but also entire muscle chains, core stability, as well as functional and explosive strength. [3] Since kettlebell exercises are complex and require athletes to have a certain level of strength and coordination, they are associated with risks of injury.
To our knowledge, no case has so far been reported in which a stress fracture of the radius occurred after intensive kettlebell training (Figure 1). Since the popularity of this type of training continues to grow, the objective of our case report is to increase understanding and awareness of this type of injury and to discuss the causes, diagnosis and treatment of stress fractures of the upper extremity.
Case presentation
A 42-year-old male soldier who had performed strength training for several years presented with pain in the right forearm to the outpatient department of the Bundeswehr Center of Sports Medicine in Warendorf, Germany.
History
Five days before, the patient had performed single-arm exercises with a 48 kg kettlebell. When he was completing the fourth set of exercises he heard a crack in his right forearm. He stopped his training and presented with moderate pain to a civilian hospital. The treating physician suspected a tear of muscle fibers and applied an ointment and a dressing. The patient was discharged home.
Clinical findings
On the day when the patient presented to our institution, he still reported moderate pain with activity but no loss of function. He had not removed the dressing during the previous days. A mild swelling, local tenderness and a hematoma that had existed for several days were noted in the distal third of the forearm.
Diagnosis
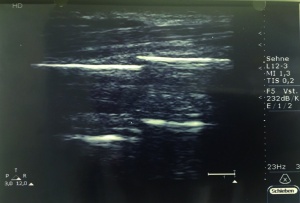
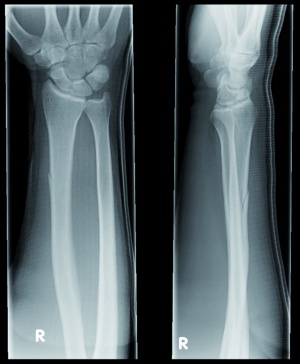
Since a tear of muscle fibers was suspected, ultrasonography of the extensor muscles of the forearm (Figure 2) was performed and suggested the presence of a fracture of the right radial shaft. The diagnosis was confirmed by radiology (Figure 3).
Treatment
A trauma surgeon from a hospital in close vicinity to the patient's home was consulted. He informed the patient about surgical and conservative treatment options and recommended conservative treatment with immobilization in a cast for approximately six weeks and radiological follow-up. The patient, however, wished to avoid the risk of delayed union after primary conservative treatment and surgical treatment following six to eight weeks of failed conservative care. He preferred a primary surgical procedure in order to quickly return to activities of daily living. Eight days after trauma, the patient underwent plate fixation in a civilian hospital in close vicinity to his home. Immediately after his hospital stay, the patient received conservative treatment consisting of lymphatic drainage and passive mobilization of the wrist and the forearm muscles at the Department of Physical Therapy of the Bundeswehr Center of Sports Medicine. Although plate fixation was found to provide stability during exercises, the patient was advised not to return to training for six weeks.
Follow-up and outcome
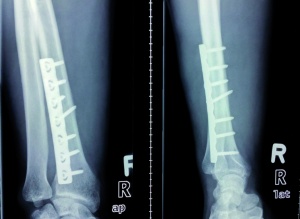
Radiological follow-up at six weeks after surgery showed complete bridging of the fracture gap with bone (Figure 4). The patient was allowed to perform gradually increasing exercises for his right forearm. The exercises were initially performed with conventional 5 kg dumbbells, the weight of which was increased every week by 5 kg. After this period, the patient resumed kettlebell training. The patient was again advised to start with a 5 kg kettlebell and increase the weight every week by 5 kg. After completion of this second six-week period of training, the patient was allowed to return to his normal training. He was advised to increase weights slowly, to take great care to perform the exercises in a technically correct manner, and to strictly limit the weight used for training.
Discussion
Stress fractures of the upper extremity are rare. For this reason, they are often omitted from the differential diagnosis during initial assessment, as in the case presented here. In 2012, MILLER and KAEDING [4] conducted a review of 70 upper-extremity stress fractures including four fractures of the radius. Similar to the response of lower-extremity bones to overloading, stress fractures of the upper extremity represent a continuum ranging from simple bone marrow edema to small micro-cracks in the cortex and ultimately to complete fractures with or without displacement. [5]
Causes of stress fractures and mechanisms of injury
Apart from torsional and shear forces, which can lead to stress fractures (especially of bones of the lower extremity), concentric and eccentric muscle contractions have been reported to cause stress reactions of the upper extremity. [4] A too rapid increase in training duration, volume, intensity and frequency that exceeds the reparative capacity of bone tissue, as well as improper technique, poor equipment, muscular imbalance and neuromuscular fatigue contribute to an increased risk of stress fractures. [5, 6] Repeated biomechanical stress on skeletal structures leads to an increased activity of bone-resorbing osteoclasts that exceeds the activity of bone-forming osteoblasts. This process temporarily weakens the affected area of bone. [7] As early as 1999, SINHA et al. [7] reported that weight bearers have an increased risk of stress fractures that occur distal to the elbow as a result of impact loading of the upper extremity. In addition to these extrinsic risk factors, which can be modified by soldiers and athletes, there are intrinsic factors (e.g. age, gender, genetic factors, and nutritional status), which can be influenced only to a limited extent. [5]
Clinical presentation
Patients with stress fractures typically describe pain that is initially associated only with repetitive loading and, when training is continued, can also occur during activities of daily living and at rest. [5, 6] Pain may be associated with local swelling, redness and local tenderness, which play a role in clinical diagnosis. When the patient in the present case completed the three sets of exercises that preceded the injury and that he performed with the same weight as the fourth set, he did not experience any signs or symptoms that indicated overloading or predicted an imminent stress fracture. In addition, the injured soldier had himself filmed while he performed the exercise that led to the injury (Figure 1) so that improper technique could be ruled out as a cause. In the case reported here, the stress fracture was probably caused by a combination of the weight (48 kg) of the kettlebell, which was held in one hand, the number of repetitions, the resulting tensile stress on bone, and the beginning of muscle fatigue.
Diagnosis
Initial diagnosis was made by ultrasound, which is not commonly used for assessing the presence or absence of a stress fracture. Magnetic resonance imaging (MRI) provides the highest combined sensitivity and specificity for evaluating early responses of bone to stress. MRI is superior to both standard radiography and computed tomography (CT) and may delineate stress reactions of bone one to fourteen days earlier than the other two modalities. [8] Bone scintigraphy too can assess stress injuries with a sensitivity of almost 100% as early as two to eight days after the onset of symptoms [9]. Increased radionuclide uptake, however, may require twelve to eighteen months to normalize, often lagging behind the resolution of clinical symptoms. [10] In the case presented here, conventional radiography demonstrated a complete fracture of the radial shaft and no other imaging modality was needed to confirm diagnosis.
Treatment
Multiple authors suggested the classification of stress fractures of the lower extremity as either high-risk or low-risk stress fractures. [11, 12] Depending on this distinction, more aggressive or less aggressive treatment is provided. High-risk fractures are defined as fractures associated with a risk of delayed union or even nonunion, a propensity for re-fracture, or long-term adverse consequences if they progress to complete fracture. [11] The majority of stress fractures of the upper extremity are classified as low-risk injuries. In 2013, MILLER and KAEDING described a classification system for stress fractures of the upper extremity on the basis of clinical and radiological findings (Table 1). This system was reported to have excellent inter-observer and intra-observer reliability [13] and can be used as a tool to guide clinicians and physical therapists in the treatment of patients as well as coaching staff in the instruction and training of athletes (Figure 5). Based on this classification system, our patient sustained a grade III stress fracture. Treatment was not provided in accordance with the treatment algorithm proposed by MILLER et al. [5] because the patient, who was enthusiastic and highly motivated to continue training, insisted on surgical fixation despite having been thoroughly informed about the risks of a surgical intervention. Without doubt, the decision to manage the fracture surgically is not without controversy since a similar outcome would have been achieved with high probability if this non-displaced fracture had been managed with conservative treatment consisting of immobilization in a cast, non-weight bearing for several weeks, and radiological follow-up.
Conclusions
Stress fractures of the upper extremity are rare but should be included in the differential diagnosis of patients reporting unusual or repetitive intense loading since current fitness trends such as kettlebell training, CrossFit and Freeletics are very popular, also among members of the armed forces. These types of sport are typically associated with a high number of load repetitions and a rapid increase in training frequency and volume and sometimes with improper technique, which are typical risk factors for stress fractures. In these cases, diagnostic imaging should be performed even in the absence of clinical signs and symptoms such as malalignment, crepitus, severe pain, swelling and hematoma formation. Ultrasonography is commonly available in Bundeswehr medical facilities and allows differential diagnoses (e.g. a tear of muscle fibers) to be ruled out rapidly, without requiring the transfer of patients to another facility and without exposing patients to radiation. In addition, ultrasound may provide initial evidence of pathological changes in bones that lie close to the surface of the body. Unit physicians should emphasize the need to perform exercises in a physiologically and technically correct manner when they give advice to athletes who start a new sport, return to sport or change their sport as well as to non-competitive fitness enthusiasts and especially coaching staff.
Key points
- Current fitness trends that involve a high training intensity and a high number of repetitions are associated with the risk of stress fractures.
- Stress fracture should be included in the differential diagnosis of patients who, with activity, experience pain of unclear origin, swelling or redness at a particular skeletal site.
- Stress fractures are also seen in less common locations (e.g. thorax and upper extremity).
- The decision to manage a stress fracture with surgical or conservative treatment should be made together with the patient and on the basis of the classification system referred to in this article.
- Physicians who give professional advice on matters related to sports and preventive medicine should emphasize the need to increase training intensity and frequency at a slow rate.
References
- Breithaupt J: Zur Pathologie des menschlichen Fußes. Med Z Berl 1855; 36: 169–171; 37: 175–177.
- Jones GL: Upper extremity stress fractures. Clin Sports Med. 2006; 25(1): 159–174 xi.
- https://en.wikipedia.org/wiki/Kettlebell (accessed on 7 July 2016)
- Miller TL, Kaeding CC: Upper-extremity stress fractures: distribution and causative activities in 70 patients. Orthopedics 2012; 35(9): 789–793.
- Miller TL, Harris JD, Kaeding CC: Stress fractures of the ribs and upper extremities: causation, evaluation, and management. Sports Med 2013: 43: 665–674.
- Teague DC: Stress fractures. In: Buchholz R, Heckman JD, editors. Rockwood and Green’s fractures in adults. Philadelphia: Lippincott Williams & Wilkins; 2012: 518–530.
- Sinha AK, Kaeding CC, Wadley GM: Upper extremity stress fractures in athletes: clinical features of 44 cases. Clin J Sport Med 1999; 9(4): 199–202.
- Banks KP, Ly JQ, Beall DP, Grayson DE, Bancroft LW, Tall MA: Overuse injuries of the upper extremity in the competitive athlete: magnetic resonance imaging findings associated with repetitive trauma. Curr Probl Diagn Radiol 2005; 34(4): 127–142.
- Roub LW, Gumerman LW, Hanley EN, et al.: Bone stress: a radionuclide imaging prospective. Radiology 1979; 132: 431– 438.
- Anderson MW: Imaging of upper extremity stress fractures in the athlete. Clin Sports Med 2006; 25(3): 489–504 vii.
- Boden BP, Osbahr DC: High-risk stress fractures: evaluation and treatment. J Am Acad Orthop Surg 2000; 8(6): 344–353.
- Boden BP, Osbahr DC, Jimenez C: Low-risk stress fractures. Am J Sports Med 2001; 29(1): 100–111.
- Kaeding CC, Miller TL: The comprehensive description of stress fractures: a new classification system. J Bone Jt Surg 2013; 95(13): 1214–1220.
Conflict of interest
The authors declare no conflict of interest in accordance with the provisions approved by the International Committee of Medical Journal Editors.
Images courtesy of
Bundeswehr Center of Sports Medicine (Figs. 1, 2 and 4)
Center of Radiology and Nuclear Medicine, K. A. Balhorn and Colleagues (Fig. 3)
Manuscript data
Submitted: 1 Feb 2016
Accepted after revision: 31 May 2016
Citation format
German:
Bender K, Holtherm C, Balhorn KA, Lison A:_ Stressfraktur des Radius durch Kettlebelltraining – ein Fallbericht.
Wehrmedizinische Monatsschrift 2016; 60(7): 218–222
English:
Bender K, Holtherm C, Balhorn KA, Lison A:_ Stress fracture of the radius as a result of kettlebell training – A case report.
Wehrmedizinische Monatsschrift 2016; 60(7): 218–222
A German version of this article you will find here.
Eine Deutsche Version finden Sie hier.
Date: 06/13/2016
Source: Wehrmedizinische Monatsschrift 2016/7

![Figure 5. Treatment algorithm for stress injuries developed by MILLER and KAEDING ([5], p. 672)](/media/gallery/339/image-1468566458.jpg)











