
Article: A. FRANKE, E. KOLLIG (GERMANY)
Recommendations for the treatment of severe burn injuries in the field – Part 2
Stabilisation, Consolidation, Transport
The complex nature of burn medicine made it necessary to divide this subject. While the first part (published in MCIF 4/11) dealt with emergency treatment of the seriously burned or of casualties with combined thermodynamic injuries in an operational context, the aim of this article is to present further procedures and the priorities of intensive ther-apy, transport to the homeland and definite surgical treatment.
Introduction
Owing to the increasing incidence of serious burn injuries within the context of wounding caused by enemy action in current operations of the German Armed Forces (Bundeswehr), a recommendation for the treatment of seriously burned soldiers in an operational environment was prepared on behalf of the Bundeswehr Advisory Group of Surgical Consultants. The most important treatment parameters are highlighted with particular emphasis on possible pitfalls. Lessons learned from our own mission experience and from the activities at the Burn Intensive Care Unit of the GER Armed Forces Central Military Hospital in Koblenz have been integrated considering existing, specific injury patterns.
Burn wounds – “developing wounds with special kinetics”
In principle, with the currently existing capabilities for first response treatment in the field, rapid transport to a prepared Role 2 or Role 3 facility and the ability to perform intensive medical transport, every soldier with a burn injury has a realistic chance of survival. However, our own experience from numerous operations and the imponderables in the area of deployment show that it is not always possible to exploit this potential at all levels. An estimation of the extent of burn injuries appropriate to the situation and, if necessary, photo documentation play a decisive role in further procedures and in the planning of treatment.
As burn wounds “develop” especially during the first few hours, they are also referred to as “developing wounds”. Each admission or transfer therefore requires an expert re-evaluation of the wound condition, and of the extent and depth of the burn injury. This does not question prior assessments and treatment. The procedure only takes into account the dynamics of the pathophysiology of this specific injury.
Following an explosion or fires in confined spaces and vehicles, lung damage combustion gas inhalation thermobaric blast injury must be assumed until the contrary is proven. In this situation or in the case of a burn injury in the face and neck area, the first priority is to secure the airways. As a matter of principle, the indication for intubation is to be liberally interpreted.
Emergency treatment is carried out according to the priorities of the established ATLS (“Advanced Trauma Life Support”) standards. In the case of burn injuries of more than 20% of the body surface area, admission to a monitoring unit should be provided for.
When assessing the burned body surface area, it is best to include all areas of at least second degree burns (IIa) (erythema and formation of blisters). The determination of the BBSA (burned body surface area) as a percentage is most reliably successful according to the “Rule of Nines”. (see also Part I)
Phases of burn shock and treatment
Burn shock or, in the case of burn injuries to over 30% of the BBSA, the regularly occurring systemic inflammatory response syndrome, occurs in phases.
The first 24 hours are characterised by a generalised capillary leak syndrome. There are massive shifts of fluids and losses of protein from the intravascular space into the interstitium and externally via the wound surfaces. It is necessary to stabilise the patient by giving him adequate volumes of isotonic crystalloids. This phase is referred to in the literature as resuscitation or the stabilisation phase.
Only with the abatement of the capillary leak after approx. 24 hours can the serum osmolarity and the oncotic pressure be normalised again through the substitution of albumin solutions and plasma. This consolidation phase extends to up to 72 to 96 hours after the injury. The aim here is to reduce the generalised tissue oedema through the reabsorption of extravasal fluid and prepare the casualty for the next phase of treatment.
The next phase of reconstruction involves the surgical treatment of burn wounds. Only a definitive reduction in the wound areas is able to interrupt the cascade of complications of the burn shock. (1) As the skin is an important immune barrier and the open wound surfaces can become contaminated with the increasing duration of treatment, it is necessary to actively influence the stabilisation and consolidation phase with regard to achieving the fastest possible reconstruction.
Blast versus burn injury
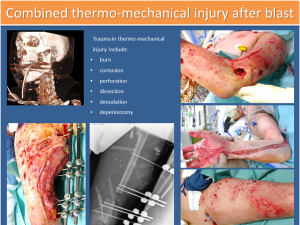 Image of combined burn injury and soft tissue damage blast
Image of combined burn injury and soft tissue damage blast
he fluid requirement within the first 24h after the burn injury can be estimated via the extent of the burns (% BBSA). In recent years, modifications to this have been introduced. (See below)
While a burn normally initially constitutes surface damage, which does not primarily affect the muscle compartments and the deeper layers of tissue, in the case of a combined thermodynamic injury, no regions and depths of the body are, in principle, spared.
Here, in addition to the burning of the surface, we find a contusion, perforation, dissection, denuding of the deeper soft tissue and, in some cases, fractures or additional injuries to the body cavities, which after the emergency medical considerations have to be included in the intensive care considerations. (see Figure 1)
The systemic burden on the organism represented by a combined thermodynamic injury is frequently underestimated. Burn injuries (to a large surface) within the framework of a blast injury are a particular polytrauma.
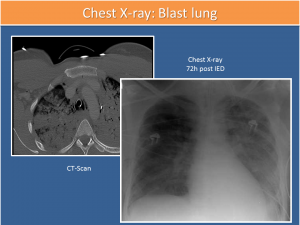 Image of blast lung
Image of blast lung
Additionally, after explosion injuries, together with primary, secondary, tertiary and quaternary injuries, with the use of explosives based on artificial fertilizers (quinary damage), there is also commonly damage to the lungs, which is known as blast lung. (see Figure 2)
It is also common that these patients display eardrum injury, so that a patient with loss of hearing after an explosion not only requires the checking and securing of the airways (additionally thorax X-ray), but also an otoscopy. The vital functions (peripheral O2 repletion) should then be monitored for 8 to 24 hours. (2;3)
Prognosis
It has already been stated that, in principle, every burn casualty in the field theoretically has a realistic chance of survival under present conditions.
Primarily survived, large-scale burn injuries are, for example, at up to 5% relatively rare at ISAF. The torso and head are relatively well protected thanks to the personal protective equipment. (see Figure 3) As regards explosion injuries among our own personnel and in the statistical analysis of operations-related data for burn injuries of other nations, the majority of cases demonstrate a pattern of damage, which exceeds the level of about 50% of damaged body surface in only 3% to 5% of cases. (4;5)
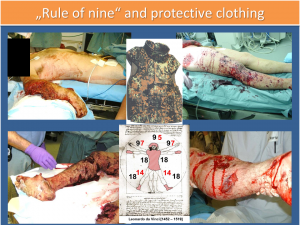 “Rule of nine” and protective clothing
“Rule of nine” and protective clothing
Here we can assume a probability of survival of around 80%. The treatment and its course are complicated by the additionally present pattern of injuries, which in most cases already of itself meets the definition of a polytrauma. (6;7)
To the extent that the casualties survive the original injuries, the primary challenge is the principle of “Nihil nocere” (“Do not further harm”).
All measures and therapeutic steps must be controlled and weighed up, so that the best possible functional result is achieved, and the casualty, after the completion of treatment and rehabilitation, either returns to service or can at least participate in the life of society without any obvious handicap and stigmatisation.
Recommendations for wound treatment: “Keep it simple”
Burn wounds are the ideal breeding ground for colonisation via an external contamination or the existing local flora. The presence of gram-positive germs, such as Streptococcus pyogenes and Staphylococcus aureus can already be demonstrated 24 to 48 hours after the injury, whereas gram-negative germs such as pseudomonas Aeruginosa, Klebsiella pneumoniae and Escherichia coli can be detected after 48 to 72 hours. (8)
As a systemic antibiotic treatment cannot prevent this colonisation and, thus far, no evidence-based benefits for the prognosis and course of the casualty can be proven for its primary application, great importance can be attributed to the cleaning of wounds within the first 6h to 8h after the wounding, with the application of topical antibiotics and antiseptics.
Following a dry dressing on the damaged area, further treatment of the burn wounds includes a thorough debridement of the surface, with, for example, moist compresses, which have been steeped in a disinfecting non-toxic solution (e.g. polyhexanide 0.02% or 0.04%). Crusts, debris, and parts of blisters are removed, cleaned and copiously rinsed.
In our view, a simple further wound treatment for the first days uses a 0.04% polyhexanide solution in a preparation as a colourless gel on a hydroxycellulose basis.
With this all burned areas of whatever degree can be dressed with polyhexanide gel and a silicone membrane (Mepitel), which does not adhere to the wound even after several days.
The aim of these colourless dressings is to keep the wounds clean and virtually or completely free of germs, avoid excessive losses of fluid through evaporation and make possible a re-evaluation of the wound condition every 6 to 8 hours within the first few days, with a regular changing of the dressing.
Considerations on intensive therapy
In principle, the seriously burned casualty requires the same intensive medical therapy as, for example, set out in national S3 guidelines for the treatment of a polytrauma (in Germany for example “Deutsche Gesellschaft für Unfallchirurgie [DGU®]”).
When treating a soldier with serious burns after a combined thermodynamic injury, we are always dealing with a special polytrauma, and correspondingly an “orchestration of the specialists”, i.e. interdisciplinary cooperation in this exceptional situation, is very particularly called for.
All the specialist disciplines involved contribute their experience from their field for the benefit of the injured soldier. The specialist on site with the most clinical experience in the specific injury pattern leads and guides the others.
Ventilation and airway management

The indication for intubation and ventilation must be liberally interpreted for those suffering from serious burn injuries. The benefits of stress reduction through sufficient analgo-sedation, a secured airway including under transport conditions and a controlled oxygenation are obvious. In individual cases, they must be weighed against the drawbacks of ventilation therapy, such as a lack of spontaneous breathing, aspiration risk, or pressure ulcers in the area of the airways and a lack of bronchial toilet.
The creation of a definitive airway is absolutely indicated in the presence of the following injury pattern:
In the case of higher-degree burn injuries (> 30% BBSA) with shifts of fluid due to the capillary leak, within the first 24 hours there is a swelling and oedema formation in all regions of the body. This must be taken into consideration carefully in particular when planning early transport with spontaneous breathing.
The ventilation therapy should include the current recommendations for lung protective ventilation. If no other injury patterns are present, which require a specific form of ventilation, tidal volumes of 4-6ml per kg of body weight are sufficient, which are achieved within the framework of pressure-controlled ventilation. (9-12)
After the initial admissions to Role 2 or Role 3, a bronchoscopy should be conducted to determine the status of the airways. Then all other measures which jeopardise maintenance of the positive endexpiratory pressure (PEEP) must be avoided and their risks always weighed critically against their benefits.
To reduce a shift of fluids into the interstitium of the lungs before the capillary leak has abated, a raised PEEP (10-12mmHg) must be applied at an early stage and maintained permanently.
The frequency of the ventilation and the FiO2 are varied corresponding to the available blood gas analyses, and normocapnia and a highly-normal oxygenation should be ensured.
If the initial PEEP is not sufficient for adequate oxygenation, further measures for recruiting lung areas must be considered. These may be an increase in the PEEP and ventilation pressure, more aggressive ventilation patterns with the generation of an intrinsic PEEP, special forms of positioning or recruitment manoeuvres.
If, due to the present injury patterns and the location and extent of the burn, a longer ventilation period is to be assumed, the early creation of a tracheostomy (dilational or surgical-open) can be still considered before repatriation. A tracheostomy reduces both the volume of dead space and the airway resistance.
In principle, the creation of the tracheostomy is easier at an earlier point in time without a swelling of the soft tissue. The clinical benefits of a longer ventilation therapy by means of a tracheal cannula have been sufficiently demonstrated. (13;14)
Nonetheless, for this optimal and progressive treatment, the personal and professional prerequisites must be present in the field. If necessary, a tracheotomy can also be conducted at a later point in time (> 72h after trauma) in the home country after the abatement of the oedema phase.
Analgo-sedation
A needs-based analgo-sedation is a prerequisite for managing pain, ventilation therapy, stress reduction and thus the stabilisation of the casualty.
In the case of ventilated victims of serious burns, in the view of the authors, the combination of ketamine, midazolam and sufentanil in the first days of treatment has proven efficacy as analgo-sedation. It is easy to control, potent and causes only mildly circulatory depression thanks to the combination. An adequately deep analgo-sedation can be achieved easily.
However, in the field an alternative regime can be adopted, with which the respective provider of the treatment has sufficient experience and the desired goals can be achieved.
Too deep sedation can be counterproductive in the first 24h, since it can leed to haemodynamic instability of the victim.
In the later phase of the treatment (4th to 5th day), the further therapeutical procedures can be adjusted according to the clinic requirements.
Here the same recommendations apply in principle as for all other intensive care patients, who profit from supported spontaneous breathing on a ventilation device, a normalisation of the sleep-wake rhythm with a daily wake-up call and titrated needs-based analgo-sedation.
Volume dose: What? - When? - How much?
In the treatment of burn victims, we distinguish, as stated at the beginning of this article, between different phases:
In the first 24 hours a capillary leak syndrome is present. In the so-called “resuscitation phase” or stabilisation phase, the volume is replaced with a crystalloid, isotonic, lactate-free infusion solution at body temperature, adapted according to need. For other infusion solutions (synthetic colloids, hypertonic saline solutions etc.), no evidence-based benefit has yet been demonstrated for those suffering from serious burn injuries. (15;16)
Different formulas are available for calculating the fluid requirement on the basis of the burned body surface area, especially within the first 8 hours after the injury. In our view, the “Parkland-Baxter formula” and the “Rule of Ten” seem to be practicable.
They are presented as alternatives in the following box:

TBSA = Total body surface area = VKO = Verbrannte Körper Oberfläche
The “Rule of Ten” consists of two steps:
First the TBSA as a % is multiplied by ten and this produces the initial infusion rate in ml/h. 100 ml are additionally infused per 10 kg of body weight over 80 kilos.
In direct comparison with the Parkland-Baxter formula, the calculated infusion volumes for patients under 40 kilos are too high, while they are lower for patients of up to 140 kg body weight. The application of this formula is simple, but requires hourly re-evaluation according to the circulation parameters and diuresis. (15;17;18)
As an increasing number of case reports in the past stated that excessive infusion of victims with serious burn injuries are exposed to an increased risk of developing abdominal compartment syndrome in the first 24h and it can be regarded as proven that a lung damaged by blast, contusion or toxic inhalation profits from a tentative volume dose, the current recommendations tend towards restrictive substitution. (19-21)
The specified formulas initially only serve to compute the fluid requirement for the first hours. The volume to be infused is then adjusted in accordance with hourly re-evaluation.
The target parameter for the needs-based provision of fluids is an hourly diuresis of 0.5-1 mg/kg of body weight. If the hourly requirement is more than 1.5 l/h, the further infusion rate should be examined critically.
Overlooked blood losses through internal injuries or e.g. pelvic fractures or underestimated damage to the lungs due to blast or inhalation can be ruled out as possible reasons for an increased volume requirement after burns in the field.
Here a blood gas analysis (BGA) is helpful. If, through significantly raised lactate values, a pathological “base excess” or acidosis, this shows a continuing reduced perfusion of the periphery or a progressive shock event, then intensified circulation monitoring by means of PiCCO® or pulmonalis catheter beyond the standard of an invasive arterial blood measurement should be discussed. (1)
It is regarded as demonstrated that invasive circulation monitoring or the repeated measurement of lactate values or the base excess does not on its own bring about any improvement in the prognosis or outcome. However, the computed peripheral resistance and the calculated cardiac output over the course of time in conjunction with the specified parameters of the BGA provide indications for the control of a differentiated volume and, if necessary, vasopressor therapy. (1;22)
The objective must be to bring the patients through the first 24 hours with the smallest possible crystalloid volume dosage and, at all events, low doses of catecholamines, with maintained sufficient perfusion and oxygenation of the periphery.
If relevant blood losses are present due to accompanying injuries, the deficit should be replaced with erythrocyte concentrates. As victims of serious burns may regularly display haematocrit values of 50% to 60% and consecutive haemoglobin values of 14-16 mg/dl in the first 48 hours, the need for oxygen carriers in the case of accompanying injuries tends to be underestimated. For these patients, a target haemoglobin value of at least 8-10 mg/dl can be assumed.
In the presence of disseminated intravascular or haemodilution coagulopathy, substitution with specific coagulation factors or plasma preparations is accordingly necessary. Normal values in repetitive monitoring of the coagulation function every 12 hours are required.
In the case of persistent circulation instability, the administration of synthetic colloidal volume replacement solutions (for example, starch or gelatine preparations) should not be considered, since they diffuse into the interstitium and it is assumed that there they encourage oedema formation after the abatement of the “capillary leak” and, furthermore, can compromise kidney function.
In these special cases, partial volume replacement with albumin solution or lyophilized plasma can be considered. An extended volume requirement of more than 1500 ml/h over 4 to 6 hours within the first 12 to 16 hours after the injury can be regarded as a threshold here. Here it is advisable to consult with an experienced burn intensive care specialist and critically weigh the need for vasopressor therapy against continued volume therapy with physiological protein solutions.
Starting from 18 to 24 hours after the injury, by administering a test dose of albumin (200 ml 20% of albumin solution) and subsequently controlling the total protein in the serum, it is possible to examine the extent to which the capillary leak syndrome persists. If there is an adequate increase in the total protein, the consolidation phase can be introduced by the controlled administration of albumin, lypholised plasma and, if necessary, erythrocyte concentrates.
After the normalisation of Hb, serum osmolarity and oncotic pressure, the reabsorption of the oedema can be introduced by a slightly increased diuresis supported by medication.
Circulation and target parameters
A non-invasive blood pressure measurement using cuffs is highly prone to error due to the formation of oedemas and is therefore insufficient. Here an arterial catheter e.g. into the radial artery or in the groin supplies more reliable measured values. Together with the arterial pressure, the heart rate over time, alongside the hourly diuresis, is a good course parameter in the stabilisation phase.
For adult patients with serious burn injuries, a heart rate of < 110 bpm can be equated with sufficient volume replacement. Frequencies over 120 bpm and a lower normal arterial pressure with an undulating pulse curve indicate a continued lack of volume.

Indicators of adequate organ perfusion in the periphery are values in the BGA normalising over time (for pH, base excess and lactates) with an hourly diuresis of more than 0.5-1 ml/kg of body weight (measured using an inserted permanent catheter with temperature probe).
The development of these parameters has to be critically reassessed on an hourly basis in the first 48 hours, since it is only thus that the infusion can be gradually reduced corresponding to the actual requirement.
Problems with volume therapy
It is known from different studies from recent years that a too-aggressive volume replacement for the most severely burned casualties is associated with an increased complication rate.
On the one hand, patients who receive excessive crystalloid volumes during the stabilisation phase more frequently develop an abdominal compartment syndrome. (1;22)
This is defined as a raised intra-abdominal pressure (greater than 20 mm HG) and the failure of an additional organ system.
This is clinically manifested by a distended abdomen, reduced pulmonary compliance, hypercapnia and a reduced diuresis.
Preventative measures are an adequate volume replacement, a corresponding positioning, analgesia and sedation as well as relief via a stomach probe and, if necessary, the prompt escharotomy of the flanks in the case of higher-degree burns.
With a demonstrated clinical manifestation and rising intravesical pressure values despite adequate therapy in repeated measurements, only the creation of an open abdomen remains as the ultima ratio. (19;20;23;24)
Furthermore, an increased oedema formation with simultaneous circular burns > 2b° is associated with a critical reduced perfusion of the extremities. This means that, in a higher proportion of cases, a complete dermatofasciotomy of the extremities is necessary for the prophylaxis of a compartment syndrome and to maintain the perfusion.
As the oedemas in the soft tissues also make the healing of skin transplants more difficult, the further operative treatment is delayed. If necessary, a necrectomy must first be carried out here and temporarily the covering of the soft tissues with a synthograft or negative pressure wound therapy (NPWT).
Kidney protection and renal replacement therapy
In principle, the objective must be to maintain self-diuresis. A passage of protein products into the renal tubules can be prevented via an alkalisation of urine through the i.v. administration of sodium bicarbonate (standard approach 10 ml/h 0.84%).
The low-dose administration of loop diuretics must be discussed critically. These are enriched in the tubular system in the event of oliguria and are then nephrotoxic. Accordingly, its use is controversial and use in the case of a prerenal kidney failure as a result of volume depletion or hypotension must be discussed critically. (25-28)
Whether the application of a CVVHDF through the removal of mediators and metabolites from the plasma offers benefits for the prognosis and outcome of the most severely burned casualties is currently being discussed and has not yet been demonstrated on the basis of evidence. This therapy should be carried out by an experienced physician at a centre and is not initially required in a Role 3.
If the CVVHDF is used, filtering should definitely be without extraction in order to maintain self-diuresis.
Nutrition and ulcer prophylaxis
Patients with serious burn injuries have a high risk of developing stress ulcers. An ulcer prophylaxis can be carried out medicinally with early enteral feeding, antihistamines and proton pump inhibitors. (29;30)
Whether antihistamines in the early phase (the first 24h) offer additional benefits for haemodynamic stabilisation, since they counteract the vasodilation through the liberation of histamines in the burned areas and prevent bronchospasms in the case of inhalation trauma, is being discussed. Also under discussion is the high-dose administration of vitamin C, but is not regarded as having been proven.
If no reflux is present, enteral feeding via a stomach tube should be initiated early. It should also be continued during transport. A high positioning of the upper body can counteract the risk of microaspiration. This position also reduces the oedema formation in the head/neck area.
Antibiotic treatment yes/no
Systematic antibiotic treatment after serious burn injuries as an infection prophylaxis is not initially indicated. It is only provided in the case of proven systemic signs of infection. (8;31;32)
Here it should be pointed out that the typical infection and sepsis criteria after extensive burns (hyperthermia, leucocytosis, tachycardia, tachypnea) can regularly occur as part of the systemic inflammatory response after a serious burn injury.
In the subsequent course an increasing fluid requirement, a falling thrombocyte count in the peripheral blood (both starting from the 3rd day after trauma) or again deteriorating lung or kidney function in the subsequent course are to be regarded as probable indications of a beginning sepsis or systemic infection. (33)
If these signs are present, more advanced diagnostics is required (clinical examination, blood cultures, U status and culture, thorax X-ray, wound swabs) and a change of all catheters, since this is always the most frequent cause of infection. Antibiotic treatment is then provided in a systemic and calculated manner according to the findings available.
For operational reasons, however, as in most cases we see soldiers with serious burns after combined thermodynamic injuries, and those soldiers also display other injuries, systemic antibiotic treatment is mandatory in these cases. It should be administered intravenously with an adequate dosage initially, for example, with a second-generation cephalosporin. The additional administration of an anaerobic offers no benefits during the course. (32)
“No gos” from a trauma surgery perspective
Various problems in the treatment of patients with serious burn injuries and additive other injuries repeatedly occur and will be again addressed here separately.
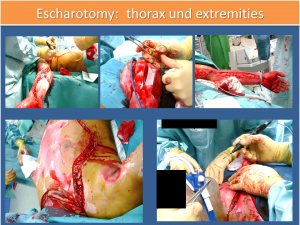 Escharotomy thorax and extremities
Escharotomy thorax and extremities
The overlooked compartment syndrome and the lack of a complete splitting of the fascia (for example, not biportal in the lower leg) is repeatedly a problem, which while it is not directly life-threatening, significantly worsens the functional outcome. In case of doubt here, whenever the suspicion is raised clinically, a splitting of the compartment at the affected extremity should be carried out. It should always be borne in mind that a compartment syndrome may arise as a result of fluid movements also at the extremities, which are primarily not burned or obviously injured.
For this reason, fractures of the extremities, especially in casualties who have additionally suffered a serious burn injury, should be sufficiently stabilised. This can be done most simply by repositioning and immobilisation with external fixators (splints).
For burn patients, dressings should be changed before the start of transport by a surgeon who is experienced in the treatment of burn injuries.
Here it is necessary to anticipate the kinetics and dynamics of the development of the wound and soft tissue finding for the transport time (8 to 12 hours). If necessary, even further compartments must be split or the escharotomy expanded in order to ensure sufficient perfusion of the extremities for the entire duration of the transport. If this expertise is not available on site, an appropriately experienced and trained surgeon should accompany the transport. (see Figure 4)
Transport logistics
Time of transport
In principle, it seems plausible to transfer a severely burned casualty to the homeland at the earliest possible point in time after the initial first response treatment in a Role 2 or Role 3 facility, since the intensive medical problems increase over time.
Within the first 24 hours, the patient isoften unstable and it is difficult to provide him with intensive medical care. Starting from 24h after trauma and with the abatement of the capillary leak, it is possible in most cases to stabilise the patient by means of specific adequate substitution. The degree of swelling of the extremities and thus the risk of developing a compartment syndrome during transport have consolidated and transfer in this phase appears to involve fewer complications.
If the patient in a Role 3 facility has a surgeon and/or anaesthetist experienced in burn treatment on site, the stay and the postponement of transfer to the second or third day after trauma can be considered and under these conditions, this is, in the opinion of the authors, the safer alternative.
Ressources
When planning the transport specific challenges must be anticipated. Sufficient amounts of body-temperature infusion solutions, blood products and modalities for airway management (e.g. bronchoscopy), ventilation (BGA analyses) and circulation monitoring must be provided for.
A sufficient number and types of catheters and access sites must be implemented in advance (obligatory fixation of all access sites by suture), which, if needed, also permit the central administering of vasopressors.
Progressive temperature loss through the evaporation of wound secretion (dry cabin air in the plane) and the absence of any possibility to control the temperature in the destroyed skin areas must be prevented by means of corresponding warming modalities (heat pads, hot air blowers, electric blankets, infrared radiators etc.).
Positioning
To the extent that the injury pattern does not argue against it, a position with a slightly raised upper body for the reduction of oedema formation in the head/neck area and for the prophylaxis of microaspiration by the ventilated casualty with the required ongoing enteral feeding also makes sense during transport.
If only individual extremities are burned, the elevated position supported from below by soft materials has proven its worth, since it reduces oedema formation locally and thus makes possible prompt further operative treatment, if necessary with early necrectomy and direct split skin grafting after repatriation.
If, owing to inhalation trauma or blast injury, the pulmonary function is so restricted that sufficient oxygenation cannot any longer be ensured even by more aggressive ventilation patterns with the generation of an intrinsic PEEP, a face-down positioning should be attempted.
In principle, in these difficult constellations prior to transport, it must be decided in an interdisciplinary manner whether transport at this point in time is practical and/or whether it can only be made possible by an additive technical procedure (e.g. extracorporeal membrane oxygenation, ECMO).
Considerations on further treatment
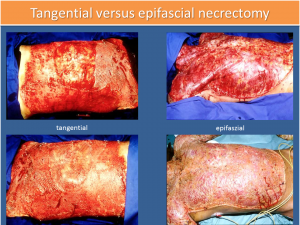 Tangential versus epifascial necrectomy
Tangential versus epifascial necrectomy
After the stabilisation of the casualty, it is necessary to remove the necroses promptly in order to reduce the systemic load by releasing mediators from the dying tissue. (Lit.)
This can be performed tangentially or epifascially. In the case of the first procedure, tissue is removed tangentially until a bleeding wound base is revealed, which can then be covered with split skin. In the case of the epifascial necrectomy, all layers are removed down to the muscle fascia. Here the cosmetic result is less good over time, but the blood losses during the operation are lower. (see Figure 5)
The term early necrectomy is not clearly defined in the literature. Depending on the publication, a necrectomy can already be called early within 72h to 96h, whereas the classic late necrectomy is a removal of burned skin after demarcation and tanning.
The extent of the necrectomy of an operation has to depend on the clinical condition of the casualty and the anaesthesiological support. Furthermore, sufficient donor area and material for temporary coverage must be available.
In the view of the authors, with an optimal interdisciplinary procedure 25% of the body area can be supplied safely in one session. The planning and execution of this treatment should take place in an institution which has enough experience in these injury patterns.
Outlook
Due to the complexity of current multinational operations and the high incidence of blast injuries and combined thermodynamic injuries, the treatment of these injury patterns has taken on international dimensions.
NATO has taken account of these challenges by establishing research task groups (RTGs), which have in the last three years met regularly to work out an expert recommendation for the treatment of specific injury patterns.
At present, a recommendation for the treatment of serious burn injuries in the field is being created. This will probably be published at the end of the year and can serve as a basis for discussion for further national efforts to treat the most severely burned casualties, including in the Bundeswehr.
While the proportion of severely burned casualties from the operations of the Bundeswehr has been very low in recent years, the proportion of wounded with complex extensive soft tissue injuries has been on the rise.
The knowledge and skills gained from the work carried out in recent years has to be consolidated and constantly applied in the clinic, adapted and introduced into training. The logistical prerequisites for the treatment of these injury patterns should be permanently reflected in the Bundeswehr in a military hospital and to an appropriate extent, one that can meet the challenges posed by current and future operations.
Considerations regarding the establishment of an intensive care and monitoring unit which, under the required climatic and hygienic conditions, permits those with complex injuries with extensive soft tissue (burn injuries, thermomechanical injuries, degloving injuries) and consecutive skeletal injuries to be treated through intensive care and operatively, are forward-looking and innovative and will meet the military medical need for training and treatment capacity.
Authors:
Lieutenant Colonel MC, Priv. Doz. Dr. med. Axel Franke, MD, PhD
Department of Trauma, Reconstructive and Orthopaedic Surgery,
Hand and Plastic Surgery, Burn Treatment
Central Hospital of the German Armed Forces, Koblenz
Rübenacherstrasse 170
56072 Koblenz
Colonel MC Priv. Doz. Dr. med. Erwin, Kollig, MD, PhD
Department of Trauma, Reconstructive and Orthopaedic Surgery,
Hand and Plastic Surgery, Burn Treatment
Central Hospital of the German Armed Forces, Koblenz
Rübenacherstrasse 170
56072 Koblenz
Date: 09/20/2018
Source: Medical Corps International Forum 4/2012











