
Article: A. TURABI, SH. C. NESSEN, D. BOEDEKER, B. BOEDEKER (USA)
Tele-Medicine for Mil.Med. Treatment Facilities
Development of a Tele-Anesthesia Preoperative Clinic
to Support Distant Military Treatment Facilities for the European Regional Medical Command
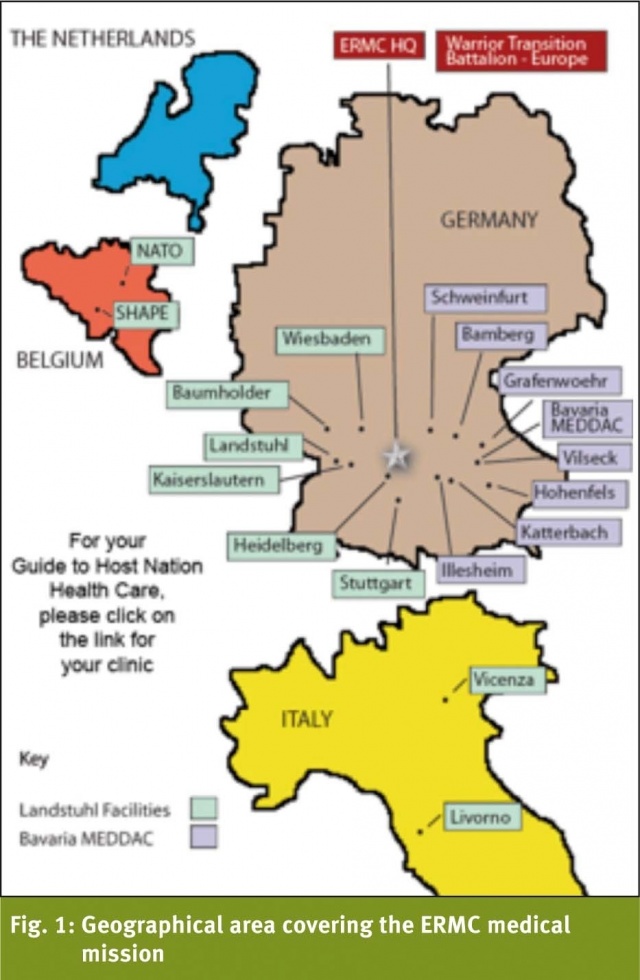
Landstuhl Regional Medical Center (LRMC) provides primary care services for more than 65,000 beneficiaries and specialty care and hospitalization for 245,000 U.S. Service Members and their Families serving in Europe. These personnel are located in Germany, Italy and Belgium (See Fig. 1). Anesthesia preoperative diagnosis/work was done by telemedicine at the distant, end user site, and significant cost savings and enhanced patient service was accomplished. A novel use of existing technologies was implemented to enhance provider and patient satisfaction and create a sustainable, user friendly system.
Introduction
The European Regional Medical Command (ERMC) supports over 20 Army heath care facilities or organizations in Belgium, Germany and Italy (figure 1). This projects mission was to exploit telemedicine to decrease patient travel and increase medical specialty reach to all parts of the ERMC command. The large geographical area covering the ERMC medical mission is shown by the map in Fig. 1. In January 2013 a virtual ENT clinic was fully implemented at Landstuhl Regional Medical Center (LRMC) increasing surgical workload significantly. A virtual anesthesia preoperative assessment clinic was subsequently established at LRMC to assist with the increased Anesthesia pre-operative workload in conjunction with satellite telemedicine sites previously established at Bamberg, Baumholder and Vilseck Army Medical Clinics for ENT telemedicine. The specific goals of the Anesthesia Telemedicine Program included:
- Expand specialty care reach to distant sites in the European Regional Medical Command
- Allow patients to be cared for within the military medical community versus seeking contract care from local civilian providers
- Prevent patient travel which was costly and removed the military member from their duty station
- Facilitate health care access to distant service members and their families.
Methods
Three pilot tele-anesthesia preoperative clinics were established at the health clinics in Bamberg, Baumholder and the Vilseck Army Medical Clinics in Germany. A virtual simulation and distance education program was developed to teach end site users how to perform basic use of camera’s and use of digital stethoscopes.
Telecommunications Methods
A goal in telecommunications support for this project was to integrate the telemedicine work flow into both the specialist (at the hub site / LRMC) and the primary care provider (at the end user distant clinics Vilseck, Baumholder, Bamberg) into their routine daily work processes. (2) This was accomplished by installing Polycom enterprise-class HD video software onto the computer workstations for the primary care providers and the specialists. This allowed the workstation that is routinely used by the providers in managing their routine medical encounters into a full videoconferencing station. Use of the provider’s existing computer for the telemedicine video conferencing prevented the need for an expensive dedicated CODEC telemedicine system and conserved limited space in the physician’s office.
Results
Distant Tele anesthesia pre-op clinic was established. Anesthesiologists at LRMC were able to do telemedicine preops to distant sites in Germany. Five telemedicine pre-ops were done successfully. This saved an estimated 1000$ in travel expenses and an estimated 25,000$ in operative expenses which would have been required if the patient had the surgery on the German economy. Patients were overall satisfied with their experience based on patient satisfaction surveys. The Anesthesiologists performing the cases were satisfied with the quality of the preoperative assessments and there were no cancelled or delayed cases reported.
Discussion
This paper describes a methodology to establish low cost Tele-anesthesia consultation capabilities between a military medical center to rural outlying clinics. The methods used consisted of a low cost approach to creating telemedicine video conferencing capabilities to support the project. Use of existing medical infrastructure, such as computers already used by physicians to perform routine medical record tasks allowed better integration of the telemedicine tasks to their usual work flow. This system can be used for low cost, effective specialty outreach from a military medical center to distant end user clinics to include deployed locations. Review of post training evaluations shows that the training and telemedicine system was well accepted by end user site medical participants. The plan at LRMC is to expand the telemedicine program to all subspecialties in order to provide consultation services to remote and deployed medical treatment facilities worldwide to provide a low cost option for quality healthcare to soldiers stationed abroad.
Acknowledgments
The authors would like to thank Gail Kuper, Department of Anesthesia, UNMC, for assistance with this project.
References: [email protected]
Date: 03/05/2014
Source: MCIF 1-14










